Laboratory Denial Management & Appeals
Reduce denial management costs through automation, prevention tools and analytics for greater efficiency, faster appeals and improved cash flow.
How We Can Help
Reduce the Complexity & Cost in Managing Denials
Denial Management helps remove the complexity and scope of managing claim denials. Our claims professionals and sophisticated technology govern health plans and the corresponding price schedules, coding combinations and the associated fee schedules from CMS. Patient visibility is gained using tools to streamline verification of insurance coverage, prior authorization and propensity-to-pay at or before the time of service. Staff errors are reduced and productivity gained with automated workflow processes. These processes identify both full and partial payer denials in real-time, and trigger appropriate actions such as appeals, corrected claims or write-offs.
Tools To Prevent Claim Denials
Verify Demographics & Insurance Coverage
Validate patient demographics and verify insurance eligibility coverage and benefits to determine patient responsibility and reduce claim denials.
Prior Authorization Sofware
Verify prior authorization requirements and medical necessity per payer policy sooner to ensure tests are approved and help protect expected revenue.
Govern Requirements, Coding & Compliance
Claims Management, combined with Denial Management, govern codes, the associated fee schedule from CMS and the contractual fees from third party payers.
Determine Propensity-to-Pay
Quickly determine a patient’s ability and probability to pay their financial responsibilities prior to the date of service.
Why Clients Choose Us
“We were able to identify one particular denial and fix the issue, which reduced the number of denied claims—meaning we eliminated the need for those claims to be reworked.”
— Director of Operations, Biodesix

Prevent & Manage Denials Efficiently
Automate Denial Management & Appeal Workflow
Denials & Appeals Management integrate with billing applications, and automatically create custom worklists and intelligent routing of denials to the appropriate user or user groups for rapid follow-up. Our solution captures full and partial denials, manages appeals at every stage with all payers, and generates appeal letter templates for immediate action. Expect to reduce future denials and rejections by improving claim accuracy, and increase efficiency and staff performance with automation—resulting in maximum reimbursement.

Data Analytics
Decision Intelligence by Quadax
Decision Intelligence by Quadax helps you gain better visibility into claim processing, payment and revenue generation data to identify contributing factors and perform real-time root cause analysis. Now you can leverage actionable data for quick resolution to more effectively reach successful business outcomes.
- Quickly capture denial history to provide actionable analytics to reduce future denials by improving initial clean claim rates.
- Review contracted claim denials to determine test criteria and if met.
- Submit multiple levels of provider or member appeals to overturn claim denials.
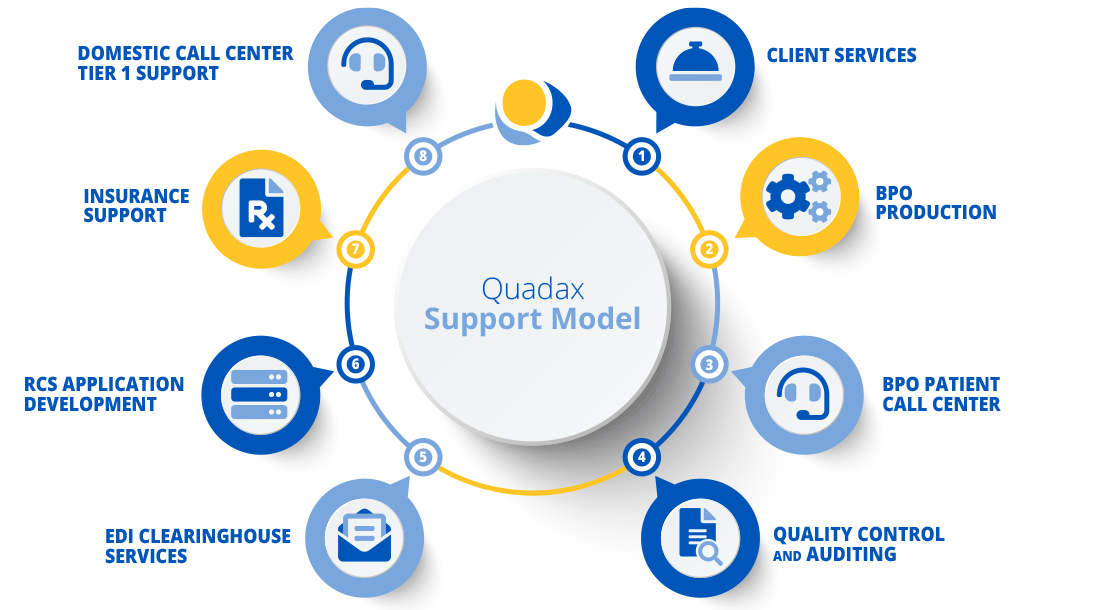
Reimbursement Consulting & Support Services
Rely on the Experts
While we offer an industry-leading purpose built RCM solution, Quadax’s greatest strength is our experience around implementation and ongoing support given our extensive history of meeting a variety of billing, reimbursement and industry challenges. The client service team is supplemented with various dedicated resources within Quadax to react quickly to client needs, not only during implementation but throughout the engagement.
