Post-Acute & Long-Term Care
Streamline medical billing, enhance visibility and control over financial operations, and mitigate compliance risks for maximum reimbursement.
The Quadax Advantage
Unified Revenue Cycle Management Solutions
Quadax’s sophisticated revenue cycle management platform—developed for Post-Acute and Long-Term Care—unifies medical billing and streamlines the process across multiple care facilities.
Our solutions are designed to partner with you in managing the entire revenue cycle, including custom development to fit your business model and goals. Using a solid financial foundation, our solutions conduct a thorough and continuous analysis of front-end to back-end revenue processes to help deliver the best possible patient care without compromising reimbursement goals.
Automated Claim Status
Claim Status is available in real‑time, batch, or automated formats, with automated workflows delivering detailed 276/277 updates, early visibility into stalled claims, and exception‑based escalation—eliminating manual portal work and improving efficiency.
Convenient FISS Connectivity
The Quadax Portal is your gateway to a wealth of information, valuable resources and customer support, and now, your staff’s gateway to Medicare’s Fiscal Intermediary Standard System (FISS).

Xpeditor
Add To Your Resources With Automation
Xpeditor automates workflow to quickly route claims to each biller based on the criteria you define, and when necessary, routes claims internally to maintain an accurate audit trail reducing the need to communicate through an external environment. Integrated workflow automation between Claims Management and EHRs and/or billing applications result in streamlined processes that improve clean claim rates, reduce administrative costs and provide the insight and control to recover expected reimbursement with speed and efficiency.

XpressBiller
Create Custom Rules & Automate Your Revenue Cycle
The path to improving clean-claim rates begins with an ounce of prevention. XpressBiller empowers you to automatically detect, assign, correct and minimize errors in real-time before the claim is released to the payer. It does this by preventing the key issues that derail claims and reduce profits.

I use the product’s reporting function a lot, and it is very easy to navigate. I love that we can create reports, apart from the ones Quadax has in their system, to fit our needs.
— Manager, Sept 2023, collected by KLAS Research

Intelligence by Quadax™
Intelligent Analytics and Reporting
Intelligence by Quadax (iQ) is our all-in-one AI framework built to streamline automation, deliver predictive insights, and optimize performance across the entire revenue cycle. From patient access to denial management, iQ empowers healthcare organizations to minimize friction, accelerate processes, and drive better outcomes.
One Solution. All Payers. Total Coverage.
ICV All-Payer
Quadax’s ICV All-Payer goes beyond eligibility verification—uniting fragmented payer data into one intelligent platform that reduces administrative burden, eliminates guesswork, and accelerates reimbursement. Whether you’re handling Medicare, Medicaid, commercial, or managed care claims, ICV empowers your team with automation and insights to drive cleaner claims, faster payments, and stronger financial performance.
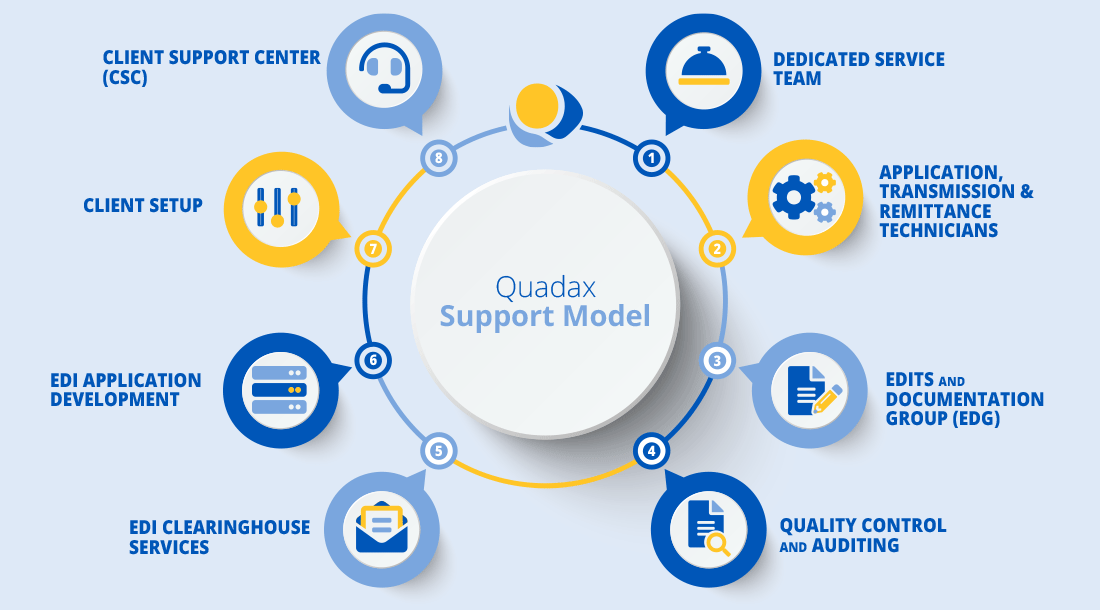
Rely on the Experts
Claims & Reimbursement Support Services
While we offer an industry-leading RCM solution, Quadax’s greatest strength is our experience around implementation and ongoing support given our extensive history of meeting a variety of billing, reimbursement and industry challenges. The client service team is supplemented with various dedicated resources within Quadax to react quickly to client needs, not only during implementation but throughout the engagement.
