Medical Billing & Follow-up Companies RCM Solutions
Streamline medical billing, enhance visibility and control over financial operations, and mitigate compliance risks for maximum reimbursement.
Move Past Recovery to Achieve Financial Resilience
Quadax goes beyond traditional claims processing. We provide comprehensive revenue cycle management (RCM) solutions that empower healthcare organizations to streamline billing, increase revenue, and minimize bad debt. By analyzing every stage of the revenue cycle, we help healthcare providers optimize their financial performance while ensuring patients receive the highest quality care.
Unified Revenue Cycle Management Solutions
Eligibility
Insurance Eligibility confirms a patient’s insurance coverage and benefits, delivering details on copays, coinsurance, and deductibles in real-time to prevent claim rejections, payment delays, or revenue loss.
Insurance Verification
Quadax’s ICV All-Payer delivers unified, real-time coverage validation across all major payers—Medicare, Medicaid (49 states), Blue Cross, Blue Shield, and Commercial—through a single platform that integrates Electronic Eligibility Verification and ICV Edit engines for maximum efficiency and control.
Automated Claim Status
Claim Status is available in real‑time, batch, and automated options, with automated workflows delivering detailed 276/277 updates directly into your system—providing early visibility into stalled claims, exception‑based follow‑up and escalation, and eliminating manual portal tracking to drive greater efficiency and automation.

Xpeditor
Integrated Workflow Automation
Quadax’s Xpeditor software streamlines workflow by directing claims efficiently to designated billers based on your criteria, ensuring a precise audit trail, and eliminating reliance on external communication channels. By integrating workflow automation between Claims Management and EHRs or billing applications, processes are optimized to enhance clean claim rates, reduce overhead costs, and empower you with the tools needed to swiftly and effectively recover expected reimbursements.

XpressBiller
Auto Fix and Scrub Claims with Custom Rules & Edits
To improve clean-claim rates, start with proactive measures. With XpressBiller, Quadax’s cutting-edge rules and editing system, automatically pinpoint, address, and reduce errors in real-time before submitting claims to the payer. By tackling the root causes that impede claims and cut into profits, you can take charge of your revenue cycle and satisfy even the most challenging payers without the need for IT involvement and at no extra cost.
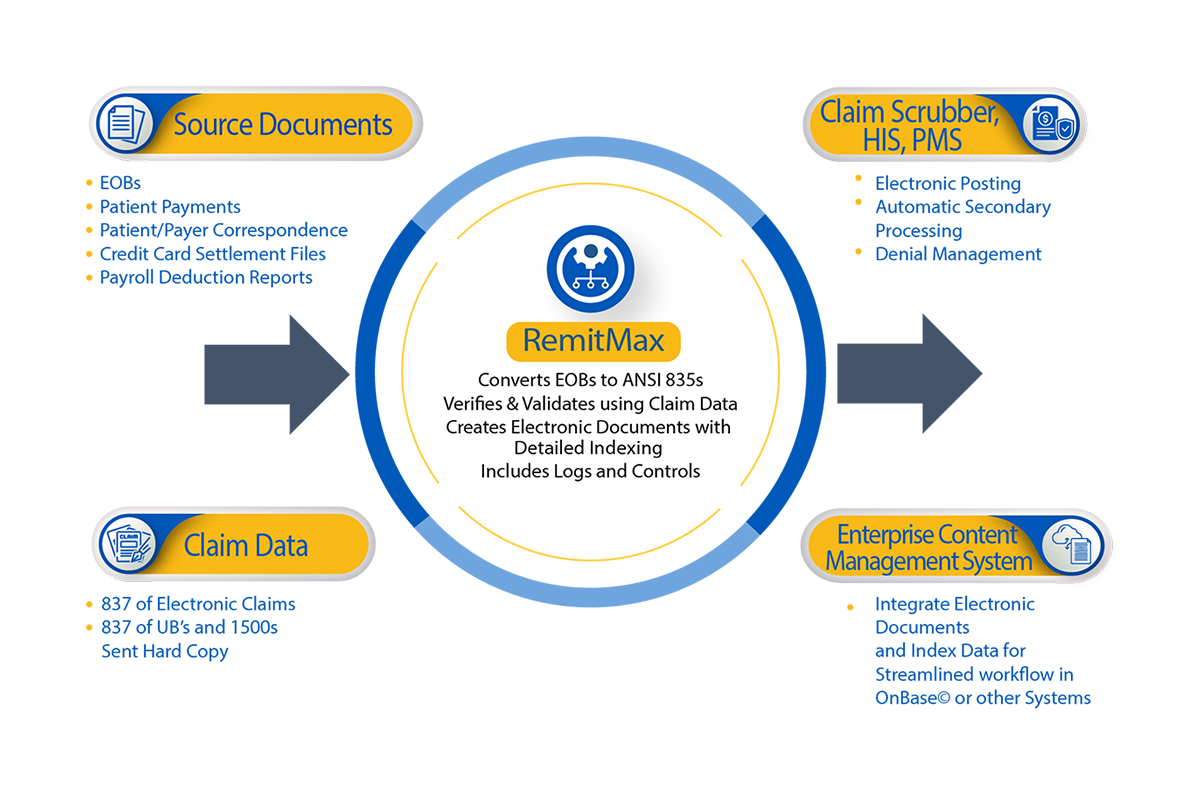
RemitMax
Eliminate Paper EOB & Correspondence Bottlenecks
Streamline your billing office workflow and saves those hard-earned dollars by eliminating paper with RemitMax by Quadax.
Adding RemitMax to your remittance management strategy allows you to get control of all your remittance and correspondence documents—even patient payments—that you or your lockbox now receive on paper. And, the 835s created by RemitMax are subject to the same automation that’s afforded within the Claims Management and Denial Management solutions, such as automated COB claims, denial management workflow and robust data analytics allowing for a more accurate picture of the entire revenue cycle.

Intelligence By Quadax™
Intelligent Analytics and Reporting
Intelligence by Quadax (iQ) is our all-in-one AI framework built to streamline automation, deliver predictive insights, and optimize performance across the entire revenue cycle. From patient access to denial management, iQ empowers healthcare organizations to minimize friction, accelerate processes, and drive better outcomes.
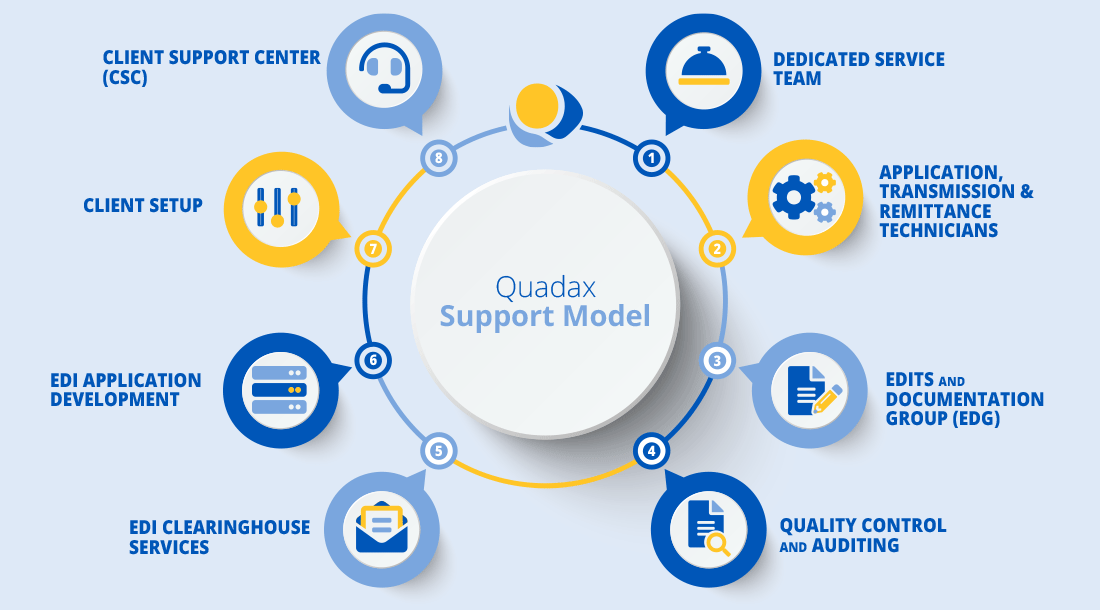
Claims And Reimbursement Support Services
Rely on the Experts
Quadax revenue cycle experts offer regular on-site visits to help with event management and resolution, ongoing training, customized reporting solutions, industry best practices, and overall issue resolution. With Quadax, you’ll experience a seamless integration of advanced technology and dependable, personalized support.
Why Our Clients Choose Us
The Ohio State University Medical Center
“With Quadax as its partner, The Ohio State University Wexner Medical Center has been able to beat its target timing for claims processing. Currently staff are processing claims in 18 days, from date of service, against a goal of 30 days.”
— Eric Long, Associate Director of Patient Accounting.
