Best Healthcare Claims Management Solution
Hospitals & Health Systems Claims Management Solutions
Five-time winner of the Best in KLAS award for Claims Management! Achieve an industry leading clean claim rate of 99.7% first-pass acceptance with payers for fast reimbursement.
99.7% first-pass acceptance with payers
Automated & Analytics-Driven Healthcare Claims Management
Quadax Claims Management is a five-time KLAS award winner, delivering 99.7% first-pass acceptance and faster reimbursement through smart automation, denial prevention, and data-driven workflows. Seamlessly integrating with your billing and EHR systems, our solution accelerates claim processing, boosts accuracy with rules-based validation, and provides actionable insights through advanced analytics.
With ongoing monitoring of payer rules by our expert RCM team, you can optimize staff resources and stay compliant—confident your claims are always aligned with the latest standards.

Xpeditor
Automate Claims Management Workflows
Quadax’s proprietary claims management software automates workflows to quickly route claims to each biller based on the criteria you define, and when necessary, routes claims internally to maintain an accurate audit trail, reducing the need to communicate through an external environment. Integrated workflow automation between Xpeditor™ and EHRs and/or billing applications result in streamlined processes that improve clean claim rates, reduce administrative costs and provide the insight and control to recover expected reimbursement with speed and efficiency.

Xpeditor is outstanding. It has very robust capabilities, and there isn’t anything that the vendor hasn’t figured out how to do with it. The system’s logic is far above the logic of any other system that I have ever dealt with. I like that I can go into the system, write my own logic, and implement it immediately. With other vendor’s systems, we have to put in a ticket and wait for weeks.
— Manager, Dec 2024, collected by KLAS Research

XpressBiller
Auto Fix and Scrub Claims with Custom Rules & Edits
The path to improving clean claim rates begins with an ounce of prevention. Prevent key issues that derail claims and reduce profits with XpressBiller. Quadax’s powerful rules and edit engine empowers you to automatically detect, assign, correct and minimize errors in real-time before the claim is released to the payer. Now you can gain more control over your revenue cycle and meet the demands of your most difficult payers without involving IT, and at no additional cost.
SafetyNet
Your Shield for Clearinghouse Resilience
Clearinghouse outages can bring your revenue cycle to a standstill. Quadax SafetyNet provides a robust backup solution, ensuring uninterrupted claims processing. Unlike generic backup systems, SafetyNet is pre-configured and deeply integrated with your existing clearinghouse, mirroring your primary system, including all your critical settings. This means your team experiences a seamless transition, with no need for new logins, workflow adjustments, or provider enrollment updates. And, it provides peace of mind, knowing your revenue cycle is secure so you can focus on patient care.

Intelligence by Quadax™
Revenue Cycle Analytics & Reporting
Intelligence by Quadax (iQ) is our all-in-one AI framework built to streamline automation, deliver predictive insights, and optimize performance across the entire revenue cycle. From patient access to denial management, iQ empowers healthcare organizations to minimize friction, accelerate processes, and drive better outcomes.

Edits & Documentation Group (EDG)
Comprehensive Library of Claim Processing Rules & Edits
Sources and related document links are embedded within Claims Management and offer full transparency into Quadax’s rules and edit logic, policies and procedures. This includes: revision history, payer explanations and links to documentation, recent updates and custom comments–allowing clients to leave their own documentation. Our comprehensive, up-to-date library of claim processing rules and edits are updated bi-weekly by our Edits & Documentation Group (EDG). The Quadax EDG team of experts, who are knowledgeable in both billing and ANSI claim requirements, reference nationally recognized sources, including AMA, CPT guidelines, Medicare Physician Fee and more.
Additional Features of Claims Management
Convenient FISS Connectivity
Quickly access FISS to make Medicare claims management easier than ever.
Electronic Claim Attachments
Support electronic claim attachment submission functionality to help free up staff resources, reduce postage costs and secure revenue faster.
Integrated Coverage Validation (ICV) All-Payer
Revolutionizes insurance verification by proactively identifying coverage issues before claims go out.
Automated Claim Status
Claim Status offers real‑time, batch, or automated access to 276/277 updates.
Real-Time Error Resolution in Epic
Epic Claims Processing
Seamlessly integrate claims generated by the Epic Resolute Billing system with all facets of Xpeditor into a single process, applying industry-leading Xpeditor claims management edits and rules for cleaner claims, while retaining workflow and response data in the Epic Resolute system. No need to wait for the next batch, Quadax returns the claim validation and response almost immediately to help you increase efficiency and accelerate reimbursement.
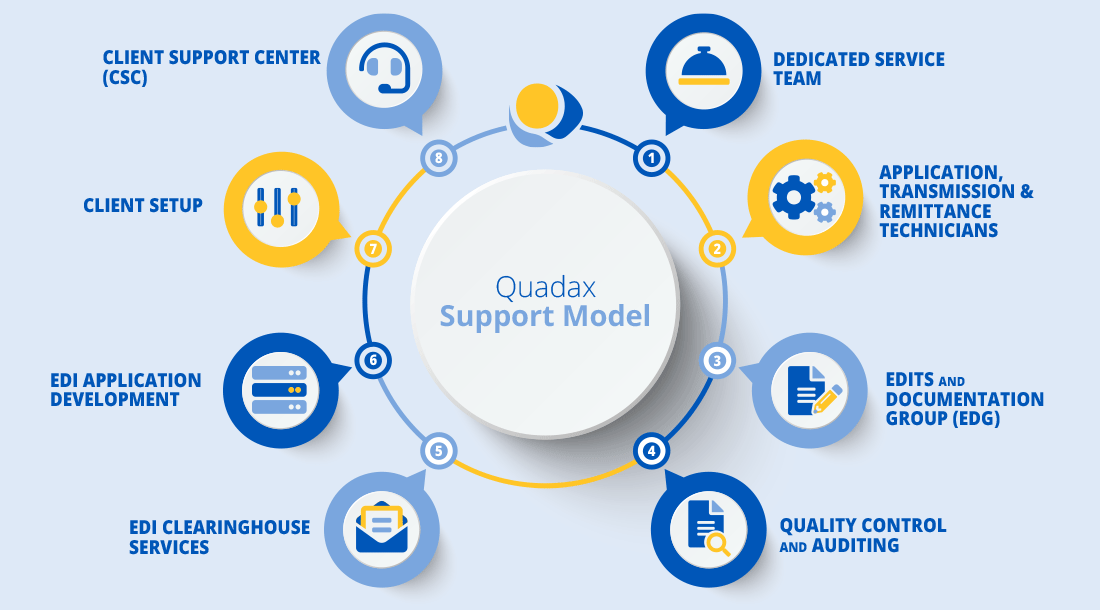
Claims & Reimbursement Support Services
Rely on the Experts
Quadax revenue cycle experts provide routine, on-site visits to assist with event creation and resolution, continued training, reporting needs, best practices and general issue resolution. Quadax provides the perfect blend of sophisticated technology with reliable, expert, personal support.
