Denial Management
Telehealth Denial Management Solutions
Reduce denial management costs through automation, prevention tools and analytics for greater efficiency, faster appeals and improved cash flow.

Denial Management
Reduce the Complexity in Managing Denials
Quadax provides easy-to-use tools for the automatic creation of custom worklists and intelligent routing of denials to the appropriate staff in your organization for rapid follow-up. Expect to reduce future denials and rejections by improving claim accuracy, and increasing efficiency and staff performance with automation. Features include:
- Automatic Creation Of Custom Worklists Eliminate manual identification and collection
- Full & Partial Denials Captured Rescue all opportunities for recovery
- Flexible Configuration Build routing rules for efficient handling
- Management Dashboards & Reports Track key performance data
- Source Documents At Your Fingertips Access key data immediately
- Appeal Letter Templates Take action swiftly and easily
Denial Workflow
Streamline claim and line level denial workflow, and receive alerts to take the appropriate action for quicker resolution and resubmission of claims.nn
Appeal Workflow
Manage the entire appeal process and create custom worklists using automation—eliminating manual identification and collection.
Audit Management
Axis provides the processes, workflow and organization you need to even the playing field with the RACs and other audit organizations.

RemitMax
Automatically convert EOBs to ANSI 835s
RemitMax by Quadax streamlines your billing office workflow and saves those hard-earned dollars by eliminating paper. Adding RemitMax to your remittance management strategy allows you to get control of all your remittance and correspondence documents—even patient payments—that you or your lockbox now receive on paper. And, the 835s created by RemitMax are subject to the same automation that’s afforded within the Claims Management and Denial Management solutions, such as automated COB claims, denial management workflow and robust data analytics allowing for a more accurate picture of the entire revenue cycle.

Decision Intelligence by Quadax
Data Analytics for Denial Management
Decision Intelligence by Quadax helps you gain better visibility into claim processing, payment and revenue generation data to identify contributing factors and perform real-time root cause analysis. Now you can leverage actionable data for quick resolution to more effectively reach successful business outcomes.
- Quickly capture denial history to provide actionable analytics to reduce future denials by improving initial clean claim rates.
- Review contracted claim denials to determine test criteria and if met.
- Submit multiple levels of provider or member appeals to overturn claim denials.
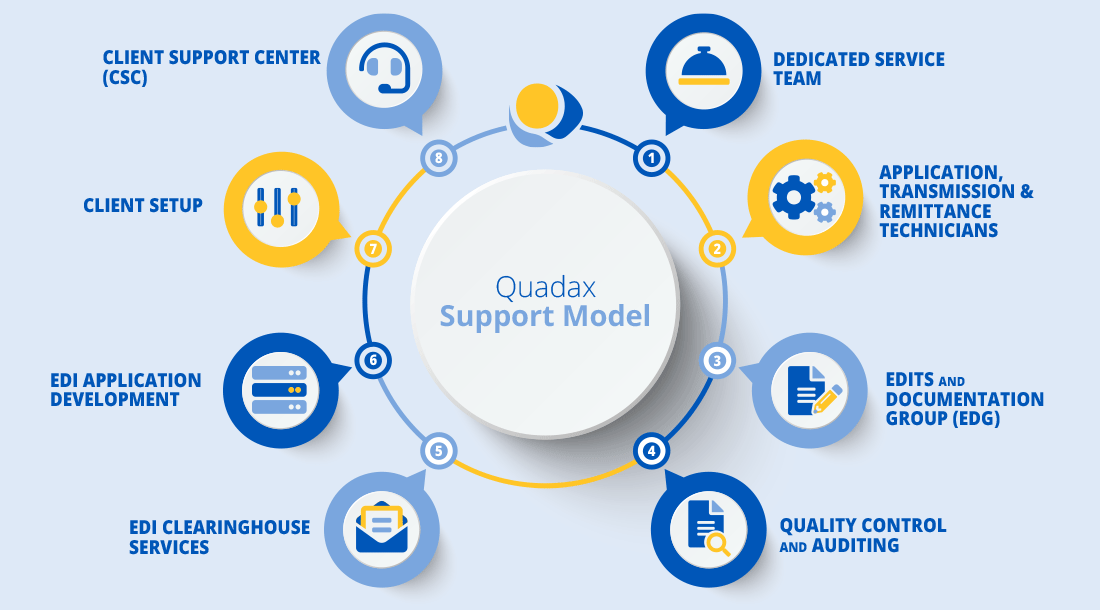
Claims And Reimbursement Support Services
Rely On The Experts
Quadax revenue cycle experts provide routine, on-site visits to assist with event creation and resolution, continued training, reporting needs, best practices and general issue resolution. Quadax provides the perfect blend of sophisticated technology with reliable, expert, personal support.
